Are you or a loved one struggling with opioid abuse and chronic pain? If so, you are not alone. It can be challenging to manage chronic pain and treat addiction simultaneously. Fortunately, mindfulness therapy has proven effective in reducing opioid use in chronic pain patients.
At Promises Recovery Ranch, we believe in using cutting-edge therapies to help our clients achieve and maintain a lasting recovery. With the help of our expert professionals, we offer a holistic approach to opioid addiction treatment, including mindfulness therapy. If you’re ready to take control of your opioid addiction while managing your chronic pain, contact us today at 1.844.876.7680.
What’s the Link Between Opioid Abuse and Chronic Pain?
Chronic pain is a form of discomfort that persists beyond the duration of the injury or illness that initially caused it. It can be caused by factors such as past injuries, nerve damage, or degenerative diseases and can significantly compromise an individual’s quality of life. For those suffering from chronic pain, the relief of symptoms is often a top priority. However, traditional pain management approaches, such as nonsteroidal anti-inflammatory drugs (NSAIDs), can be ineffective, and long-term use of opioids is sometimes necessary.
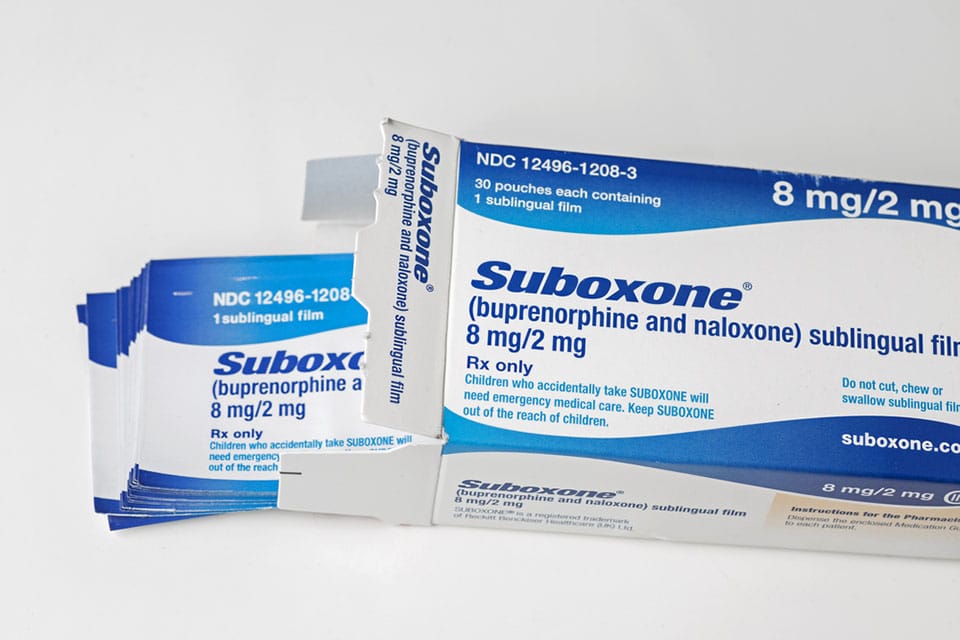
Unfortunately, long-term opioid use can severely affect an individual’s physical and mental health, leading to addiction and numerous other consequences. Opioid abuse has reached epidemic proportions throughout the country. Many individuals who initially began taking the medication as prescribed by their healthcare professionals have developed a dependency on it. Individuals sometimes turn to street drugs like fentanyl when the opioid prescription is no longer available.
One of the most significant risks associated with chronic pain and opioid abuse is the mutual reinforcement of the two conditions. Those who suffer from chronic pain are more prone to developing opioid use disorders due to the reduction of long-term relief from opioids. Individuals with drug dependency issues may develop opioid-induced chronic pain conditions. Chronic pain and opioid addiction is a dangerous cycle that is difficult to break out of without undergoing specialized addiction treatment.
Mindfulness Therapy and Opioid Abuse
Mindfulness is a mental technique that allows individuals to focus on the present moment and promotes awareness of physical sensations, thoughts, and emotions. Practices such as meditation and breathing exercises can decrease chronic pain symptoms and reduce the need for opioids. Additionally, mindfulness therapy can help patients manage stress, anxiety, and depression, which often contribute to opioid dependence.
Evidence suggests that mindfulness therapy can effectively treat opioid addiction, specifically in chronic pain patients. Studies have demonstrated that practicing mindfulness therapy can significantly reduce opioid use and improve overall quality of life.
Find Mindfulness Therapy for Opioid Addiction at The Ranch
At Promises Recovery Ranch, we offer mindfulness therapy as part of our addiction and mental health treatment programs. Our experienced team can work with chronic pain patients to develop a mindfulness practice to reduce their reliance on opioids and improve their overall well-being.
At Promises Recovery Ranch, we understand the unique challenges that chronic pain patients face when seeking addiction and mental health treatment. Our holistic approach to care includes individualized treatment plans that integrate evidence-based therapies such as mindfulness therapy. We prioritize our client’s physical, emotional, and spiritual well-being and offer a supportive and compassionate environment that promotes the recovery of all people.
If you or a loved one is struggling with opioid addiction and chronic pain, contact Promises Recovery Ranch. Our team of experts can answer your questions and guide you toward the best treatment options for your needs. Contact us today at 1.844.876.7680 or online to learn more about our mindfulness therapy, opioid addiction, and how we can help.